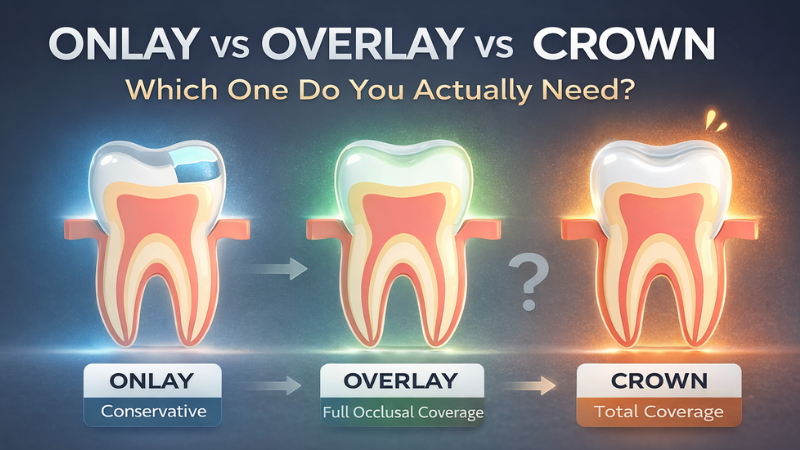
Choosing between an onlay, an overlay, and a full coverage crown can feel more complicated than it needs to be.
Many general dentists hesitate when planning indirect restorations because they are weighing up tooth preservation, material strength, longevity, occlusal forces, and patient expectations all at once. The result is often second guessing and overthinking.
The truth is that the decision does not need to be overwhelming. When you understand the biological principles behind minimally invasive dentistry and apply a structured framework, choosing between an onlay, an overlay, and a crown becomes clear and predictable.
This article breaks down the differences in a practical, evidence informed way and connects directly to the philosophy taught in the RipeGlobal Minimally Invasive Indirects Bootcamp.
Understanding the Core Difference
Before comparing indications, it is important to define what each restoration actually replaces.
What Is an Onlay?
An onlay is a laboratory fabricated indirect restoration that replaces one or more cusps and part of the occlusal surface of a tooth. It does not cover the entire occlusal table.
Onlays are typically indicated when:
- There is significant loss of tooth structure due to caries or fracture
- One or more cusps are undermined
- The remaining tooth structure is still largely intact
- The aim is to preserve as much enamel as possible
Onlays allow cuspal coverage without removing healthy tooth structure unnecessarily. When bonded correctly, they can reinforce weakened cusps while maintaining structural integrity.
What Is an Overlay?
An overlay extends further than an onlay. It replaces the entire occlusal surface and usually all cusps, but it does not extend circumferentially to full axial coverage like a crown.
Overlays are often indicated when:
- There is generalized occlusal wear
- Multiple cusps are compromised
- The occlusal table is structurally weak
- The goal is complete cuspal protection while remaining conservative
Overlays are particularly valuable in cases of erosion, attrition, or cracked tooth syndrome where full occlusal coverage is required but aggressive axial reduction is not biologically justified.
What Is a Full Coverage Crown?
A crown replaces the entire coronal portion of the tooth. It typically involves circumferential reduction of axial walls and complete coverage of all cusps.
Crowns are generally indicated when:
- There is extensive structural compromise
- Existing restorations are failing across multiple surfaces
- There is limited remaining enamel for predictable bonding
- There is a need for significant alteration of tooth form
Crowns provide maximum coverage and protection but at the cost of greater removal of tooth structure.
The Biological Question: How Much Tooth Do You Really Need to Remove?
One of the most common clinical mistakes is defaulting to crowns out of habit rather than necessity.
Research consistently supports the principle of preserving enamel whenever possible. Enamel provides the most reliable substrate for adhesive bonding. The more enamel that remains, the more predictable the bond strength and long term outcome.
When you reduce a tooth for a crown, you are committing to circumferential removal of enamel and dentine, even in areas that may not require it structurally.
In contrast:
- Onlays protect compromised cusps selectively
- Overlays provide full occlusal protection without unnecessary axial reduction
- Crowns remove more tooth structure but may be essential in certain situations
The key is not asking, “Which restoration is strongest?” but rather, “What is the minimum intervention required to restore function and longevity?”
This philosophy sits at the core of minimally invasive indirect dentistry.
A Practical Decision Framework
To simplify decision making, consider three key questions.
1. How Much Sound Enamel Remains?
If there is substantial circumferential enamel remaining, adhesive indirect restorations such as onlays and overlays are often ideal.
If enamel is minimal or margins would predominantly sit on dentine, a crown may provide more predictable retention.
2. Are the Cusps Structurally Compromised?
If only one or two cusps are weakened, an onlay is often sufficient.
If all cusps are at risk or there is widespread occlusal wear, an overlay may be more appropriate.
If axial walls are severely compromised or previously heavily restored, a crown may be indicated.
3. What Are the Functional Demands?
Occlusal load matters.
Patients with bruxism, parafunctional habits, or heavy occlusion require careful material selection and design. However, this does not automatically mean a crown is required.
Modern adhesive ceramic and composite materials, when used correctly, perform predictably under occlusal load when bonded to adequate enamel.
The decision is less about force alone and more about how that force is distributed across remaining tooth structure.
Why Overthinking Happens
Many dentists overthink indirect restoration planning because:
- Preparation design feels inconsistent
- Occlusal reduction depth is unclear
- Margins feel unpredictable
- There is fear of post operative sensitivity
- Bonding protocols are not second nature
When preparation principles are not systemised, every case feels like a new puzzle.
That uncertainty often pushes clinicians toward crowns simply because they feel familiar.
The solution is not more theory. It is structured, repeatable workflows.
The Minimally Invasive Indirects Approach
The Minimally Invasive Indirects Bootcamp by RipeGlobal was designed specifically to remove the confusion around onlays, overlays, and crowns.
The focus is on:
- Clear preparation guidelines
- Defined reduction protocols
- Occlusal assessment frameworks
- Adhesive workflows that minimise post operative sensitivity
- Step by step case planning
Instead of debating restoration type in isolation, clinicians are taught to evaluate structural integrity, enamel availability, occlusion, and long term biomechanics in a logical sequence.
The goal is confidence through clarity.
Common Clinical Scenarios
Large Failing Amalgam With One Undermined Cusp
In this case, an onlay is often ideal. It protects the compromised cusp while preserving intact enamel on other surfaces.
A crown would remove healthy structure unnecessarily.
Worn Posterior Tooth With Generalised Attrition
If occlusal surfaces are flattened and all cusps are affected, an overlay can restore occlusal anatomy while remaining conservative.
Full axial reduction may not be required.
Heavily Restored Tooth With Minimal Remaining Enamel
If there is limited enamel for bonding and significant structural loss, a crown may provide the most predictable outcome.
The restoration choice should always match the biological reality of the tooth.
Long Term Predictability and Evidence
Clinical studies show that bonded indirect restorations, when properly indicated and executed, demonstrate high survival rates comparable to crowns in many posterior cases.
Success depends on:
- Adequate enamel bonding
- Proper isolation
- Appropriate material thickness
- Occlusal management
The restoration type itself is not the determining factor. Case selection and execution are.
Stop Defaulting. Start Deciding.
Choosing between onlays, overlays, and crowns does not need to feel complex.
When you shift from habit based planning to biology based planning, the decision becomes straightforward.
Ask:
- What is structurally compromised?
- What enamel remains?
- What is the minimum intervention required?
Indirect restorations should feel conservative, logical, and predictable.
If they currently feel stressful or inconsistent in your hands, it is not because they are inherently complicated. It is usually because the workflow has not been standardised.
That is exactly what modern minimally invasive indirect training aims to solve.
Onlays, overlays, and crowns are not competing options. They are tools.
The right restoration is the one that restores strength and function while preserving as much natural tooth as possible.
When you apply structured principles, preparation guidelines, and adhesive protocols consistently, you stop overthinking and start planning with confidence.
For dentists looking to refine their indirect restorative decision making and build predictable, conservative workflows, structured education such as the Minimally Invasive Indirects Bootcamp provides a clear pathway from uncertainty to clarity.
Because in modern dentistry, precision should feel intentional, not complicated.